This blog was updated in April 2026 to add expanded content on bulging disc vs herniated disc.
| A bulging disc occurs when the soft inner layer of a spinal disc pushes outward against the outer layer without breaking through. A herniated disc occurs when that outer layer tears or cracks and the inner material leaks out. Both can press on nearby nerves and cause back pain, leg pain, or arm pain. A slipped disc is simply a casual term for a herniated or ruptured disc — it refers to the same condition. The difference matters clinically: herniated discs are more likely to cause pain because the leaked disc material can directly irritate the nerve root. |
If you are suffering from back pain or leg pain caused by your spine, you may wonder if there is a difference between bulging disc vs. herniated disc. These two terms are often used interchangeably because they are fundamentally the same thing: damage to a disc that presses on a nerve and causes pain in the back and/or the legs (or arms, if the damaged disc is in the neck).
While these two conditions are similar, they are not technically the same — although that probably doesn’t matter to you if you are experiencing pain from either of these conditions! Let me explain more about bulging disc vs. herniated disc and the best treatment options for both.
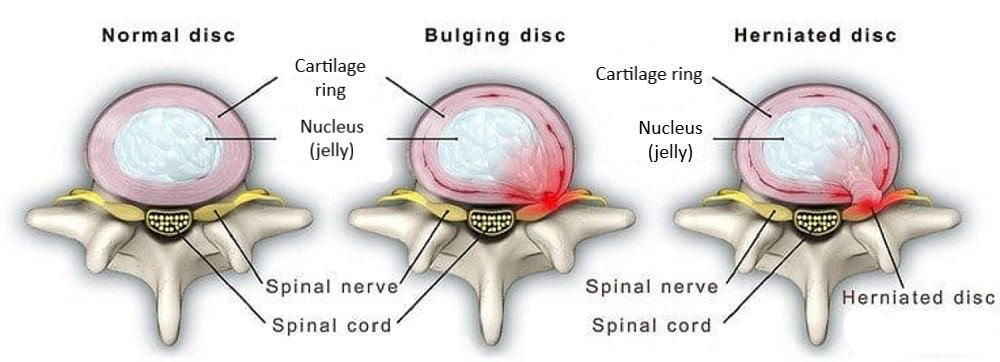
What’s the difference between bulging disc vs. herniated disc?
The main difference between bulging disc vs. herniated disc is the extent of damage to the disc. Think of your discs as jelly donuts that lie next to your vertebrae, with your spinal nerves running between the two. A bulging disc results when the jelly-like inner layer of the disc pushes against the outer layer of the disc, which then pushes on the nerve and can cause pain. A herniated disc occurs when the outer layer of the disc tears or cracks and the inner layer leaks out and pushes on the disc, also potentially causing pain.
Both bulging discs and herniated discs are types of degenerative disc disease. Disc degeneration is caused by injury, aging, regular physical labor, or sitting or standing for extended periods. Growing older is the most common cause of bulging and herniated discs. In fact, everyone over the age of 40 has some form of degenerative disc disease, according to the Arthritis Foundation.
While most adults will experience disc degeneration, not everyone will experience pain. If a bulging disc or a herniated disc causes symptoms, most people will experience pain radiating in the back and/or down the leg or arm (depending on where the disc problem occurs). The pain can be steady, or it could increase when sitting and decrease when walking. Some people also may experience muscle weakness, spasms, or tightness. In my experience, a herniated disc is more likely to cause pain because there is an actual tear in the outer layer of the disc.
Bulging disc vs. herniated disc are commonly used interchangeably as they are very similar. Only imaging can distinguish between a bulging disc and herniated disc. MRI, CT scans, and X-rays can be effective in identifying bulging discs and herniated discs.
Comparison of Spinal Disc Problems
Bulging DiscWhat happens: Inner layer pushes against outer layer; outer layer remains intact Causes pain? Sometimes, but not always Diagnosed with: MRI or CT scan Typical treatment: Conservative first: rest, PT, injections |
Herniated DiscWhat happens: Outer layer tears; inner material leaks out Causes pain? Likely as leaked material can irritate nerve root directly Diagnosed with: MRI Typical treatment: Conservative first; injections; surgery if needed |
Slipped DiscWhat happens: Casual term for herniated or ruptured disc (same condition) Causes pain? Likely as leaked material can irritate nerve root directly Diagnosed with: MRI or CT scan Typical treatment: Conservative first; surgery if needed |
Degenerative Disc DiseaseWhat happens: Gradual breakdown of disc height and integrity over time as you age Causes pain? Usually, due to “bone on bone” arthritic changes or nerve compression Diagnosed by: MRI, CT or X-ray Typical treatment: Conservative; surgery reserved for severe cases |
What does a bulging or herniated disc feel like?
The symptoms of a bulging or herniated disc depend on where in the spine the disc problem occurs and whether it is pressing on a nerve.
Lumbar (lower back) disc symptoms:
A lumbar bulging or herniated disc is the most common type. It can cause low back pain, pain that radiates down one leg (sciatica), numbness or tingling in the leg or foot, and in some cases weakness in the leg or foot. The pain often worsens when sitting for long periods and may improve with walking.
Cervical (neck) disc symptoms:
A cervical disc problem can cause neck pain, pain that radiates down one arm (cervical radiculopathy), numbness or tingling in the hand or fingers, and weakness in the arm or grip. In rare cases involving severe cervical disc herniation, patients may experience symptoms in both arms or legs — a sign of spinal cord compression (myelopathy) that requires urgent evaluation.
As noted above, a herniated disc is more likely to cause radiating nerve pain than a bulging disc, because the leaked inner material is chemically irritating to nerve tissue. However, both conditions can be painful, and the intensity of pain does not always reflect the severity of the damage shown on imaging.
What are treatments for bulging disc vs. herniated disc?
Most of the time, bulging disc and herniated disc follow the same course of treatment. At Neurosurgery One, we almost always begin with conservative treatment, such as steroid injections, unless you are experiencing any red flag symptoms that require immediate intervention. In fact, our spine team includes interventional pain management physicians who specialize in non-surgical treatments for spine pain, so you don’t even have to leave our practice to get the care that’s best for you.
If surgery is necessary, bulging disc surgery is most often a minor surgical invention. A microdiscectomy or endoscopic discectomy are the most common surgeries for bulging discs. These minimally invasive spine surgeries remove the protruding part of the disc that is compressing the nerve.
A patient with a herniated disc also can be treated with a microdiscectomy, but they may need more invasive surgical intervention, particularly if the herniated disc is causing loss of bowel or bladder function or pain into the leg. Like a microdiscectomy or endoscopic discectomy, a traditional discectomy removes the damaged part of the disc; however, it is performed through a larger incision.
In a study of patients who underwent a microdiscectomy, endoscopic discectomy, or a laminectomy/laminotomy with discectomy for their lumbar disc herniation, 79% had good or excellent results. For patients who underwent an anterior cervical discectomy and fusion (ACDF) for disc herniation in the neck, or cervical area of their spine, upwards of 95% self-reported success.
What is the typical treatment pathway for a bulging or herniated disc?
- Rest, ice/heat, and over-the-counter pain medication like ibuprofen (first 1–2 weeks)
- Physical therapy and targeted stretching (weeks 2–6)
- Spinal injections — epidural steroid injections, facet joint injections, or nerve blocks — if pain persists after 4–6 weeks of conservative care (administered by our interventional pain management physicians)
- Spine surgery consultation if symptoms have not improved after 6–8 weeks of conservative and injection-based treatment, or sooner if red flag symptoms are present
- Minimally invasive surgery (microdiscectomy or endoscopic discectomy) if surgery is necessary — most patients go home the same day.
What are the differences between slipped disc vs. herniated disc?
In addition to bulging disc vs. herniated disc, you also might wonder about slipped disc vs. herniated disc. These are actually one and the same. Slipped disc is a more casual term for herniated or ruptured disc. Slipped disc may be used more frequently for patients with spondylolisthesis, which is when a vertebra (the bone portion of your spine) slips forward over the vertebra below it.
The treatment for slipped disc is the same as it is for a bulging disc or herniated disc. Ice, rest, and pain medications are usually the first line of treatment, and some patients may progress to physical therapy if necessary. Upwards of 90% of patients with slipped disc or herniated disc do not need surgery, according to a research analysis.
Can a bulging or herniated disc heal on its own?
Yes — in most cases, a bulging or herniated disc will improve significantly without surgery. The disc itself does not fully regenerate, but the body can reabsorb some or all of the herniated material over time, reducing or eliminating pressure on the nerve. Studies have shown that larger herniations — which cause the most symptoms — are also the most likely to be reabsorbed by the body. Many patients find that their symptoms resolve substantially within six to twelve weeks of conservative treatment, including rest, physical therapy, anti-inflammatory medications, and spinal injections.
Surgery is not a requirement for most patients with a bulging or herniated disc. At Neurosurgery One, more than 90% of our patients with disc conditions are treated successfully without surgery. However, there are situations that require prompt medical evaluation — and some that require urgent surgery. If you experience loss of bladder or bowel control, rapidly progressing leg or arm weakness, or severe unrelenting pain, seek medical care immediately. These symptoms can indicate serious nerve damage that must be addressed quickly to prevent permanent injury.
When should I seek treatment for bulging disc vs. herniated disc?
The vast majority of patients benefit from conservative treatments. If you believe you have a slipped, herniated, or bulging disc and have symptoms that are interfering with your daily life, you should first see your primary care provider. In most cases, ice, rest, pain medications, and physical therapy will likely help alleviate your pain and symptoms. If your condition does not improve in 6-8 weeks, your doctor will most likely refer you to a neurosurgeon for a spine consultation where we can discuss next steps such as spinal injections vs. surgery.
If you have loss of bladder or bowel function, leg or arm weakness, or severe pain, you should seek medical care immediately. This can indicate severe damage to your spine or nerve, and your condition must be treated immediately to avoid long-term damage.
How long does it take to recover from a bulging or herniated disc?
Recovery time depends on the severity of the disc problem and the treatment path.
-
- Conservative recovery (no surgery): Most patients with a bulging or herniated disc who are treated conservatively experience meaningful improvement within six to twelve weeks. Some patients recover faster; others with significant nerve involvement may take three to six months to fully resolve symptoms.
- After microdiscectomy (minimally invasive surgery): Most patients go home the same day and return to light activity within two weeks. Many resume desk work within one to two weeks and more physical activity within four to six weeks. Full recovery, including return to heavy labor or high-impact exercise, typically takes six to twelve weeks.
- After ACDF (for cervical disc herniation): Most patients resume light activity within two to four weeks. Full recovery including return to physically demanding work or sport typically takes three to six months.
See a Denver spine specialist at Neurosurgery One
If you have been living with back pain, neck pain, or leg pain that has not improved with home care, the spine specialists at Neurosurgery One can help determine whether you have a bulging disc, herniated disc, or another spinal condition — and what the best treatment path is for your specific situation.
Neurosurgery One is the largest independent neurosurgery and spine practice in Colorado, with six locations serving the greater Denver metro area: Littleton, Lakewood, Denver (Porter), Parker, Lone Tree, and Castle Rock. Our practice includes both interventional pain management physicians who specialize in non-surgical treatments including spinal injections and neurosurgeons who specialize in minimally invasive spine surgery. This means you can get coordinated, comprehensive spine care without being referred between separate practices.
All new patients can be seen within five business days — often quicker. Request an appointment online or call 720.638.7500.
FAQs About Bulging Disc vs. Herniated Disc
Is a bulging disc the same as a herniated disc?
Not exactly. Both involve damage to a spinal disc, but a bulging disc occurs when the disc’s outer layer remains intact and simply bulges outward under pressure. A herniated disc occurs when the outer layer tears and the soft inner material leaks out. A herniated disc is more likely to cause significant nerve pain because the leaked material can directly irritate the nerve root.
Can a bulging disc heal without surgery?
Yes, in most cases. The body can often reabsorb herniated or bulging disc material over time, reducing or eliminating nerve pressure. The majority of patients — more than 90% — improve with conservative treatment including physical therapy, rest, anti-inflammatory medication, and spinal injections, without ever needing surgery.
What is the difference between a slipped disc and a herniated disc?
There is no clinical difference. “Slipped disc” is a common informal term for a herniated or ruptured disc. The disc does not literally slip out of place; the term refers to the same condition as a herniated disc. Treatment is identical.
How do I know if my disc is bulging or herniated?
You cannot tell from symptoms alone — only imaging can make that distinction. An MRI is the most accurate test for diagnosing disc problems, including the location of the disc damage and whether a nerve is being compressed. Your physician will typically order imaging if your symptoms have not improved after several weeks of conservative treatment.
When should I see a doctor for a bulging or herniated disc?
You should see a physician if your back or neck pain has not improved after six weeks of home treatment, if your pain is radiating down your leg or arm, or if you have numbness or muscle weakness. Seek emergency care immediately if you experience loss of bladder or bowel control, sudden severe pain, or rapidly progressing weakness in your arms or legs.
| Dr. Zain Allison, MD, is a neurosurgeon and spine surgeon serving patients in our Denver and Lakewood clinics. Dr. Allison specializes in cranial and spinal neurosurgery, including trauma. Dr. Allison obtained his medical degree at the University of Hawaii John A. Burns School of Medicine. He completed his neurosurgery residency at the University of Texas Medical Branch in the Texas Medical Center, where he treated patients at five hospitals, including a Level 1 Trauma Center, a comprehensive stroke center, and a Level IV NICU. Dr. Allison is the founder of a non-profit organization, “Gratia Servo,” that helps fund access to emergency medical care in Madagascar and Uganda. |